-
Cosmedocs| Non Surgical
-
COSMESURG| Surgical
-
HARLEY STREET| Skin Care
FORMULATIONS -
| Skin Bar Clinic
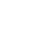 GLOW & GO
GLOW & GO
Botox in pain management
Long before, the use of Botulinum toxin started for treating cosmetic conditions; it has been used for treating various clinical disorders related to muscular malfunction by temporarily inducing relaxation in skeletal muscles. In the management of pain, the use of Botulinum toxin has shown analgesic effects by decreasing the hyperactivity of muscles, but studies now suggest that Botox could have a direct analgesic effect that is different from its effects on neuromuscular activity.
The benefits of Botulinum toxin type A in relieving chronic migraines show no direct concordance between muscle relaxation and improvement in pain in neuromuscular conditions1. This suggests that mechanism of action of botulinum toxin in relieving pain may not be strictly due to muscle relaxation. Other similar research findings2 3 have increased the interest of researchers towards identifying the possible mechanism through which Botulinum toxin type A may work to reduce pain.
Mechanism of pain transmission
There are two types of afferent nerves or primary nociceptive nerves that are responsible for pain signals transmission to the central nervous system which includes;
- Delta fibres that are responsible for mediating sharp and pricking pain
- C fibres that are responsible for mediating slow, burning pain
The dorsal root ganglia is a house to the cell bodies of these neurons where they transmit single process that branches out to innervate periphery nerves as free nerve endings (nociceptors- pain sensory organs) and also to innervate the central nervous system by synapsing the neurons located in the dorsal horn of spinal cord. The trigeminal neurons (A delta and C fibres) are responsible for pain detection in the face and head. These cell bodies of these neurons are located in the trigeminal ganglion while their axon synapse is located in the brain stem. The type C fibres of trigeminal neurons release substance P, somatostatin and other types of neuropeptides from central as well as peripheral terminals. These peptides are responsible for mediation of pain and inflammation.
How Botulinum Toxin Type A works?
Studies have indicated that Botulinum toxin type A inhibits the release of substance P from the cultured dorsal root ganglion neurons4-5. The primary nociceptive afferents (C nerve fibres) releases substance P which is a neurotransmitter. Also, calcitonin gene-related peptide (CRGP), inflammatory neuropeptide which is released from trigeminal ganglion cell, has been postulated to have a pathogenic role in stimulating pain. Botulinum toxin type A has been found to reduce the stimulation but not the basal release of calcitonin gene-related peptide (CRGP) from cultured trigeminal ganglia neurons6 7.
Botulinum Toxin type A elicits muscle relaxation by inhibiting the release of acetylcholine from alpha and gamma neurons. Additionally, several animal studies8 9 10 11 have indicated that botulinum toxin has antinociceptive effects. The possible Botulinum toxin type A mechanism through which it works in reducing pain may involve inhibition of pain causing neuropeptides and a direct reduction in the pain nerve peripheral sensitization which indirectly reduce central sensitization correlated with chronic pain.
Recent studies12 13 14 have suggested the efficacy of Botulinum toxin type A in treating postherpetic neuralgia which makes it likely to be effective for trigeminal neuralgia and post-traumatic neuralgia. A research study was conducted to explore the direct analgesic effects of Botulinum toxin type A in chronic neuropathic pain15. The results of the study showed that botulinum toxin type A had direct analgesic and persistent effects on a spontaneous intensity of pain for 2-14 weeks following the injections. Botox also reduced allydonia to brush as well as cold pain threshold without having affected on the perception of thresholds. These effects were independent of its effects on muscle movements. Another research study found that administration of Botox injections significantly reduced pain in postherpetic Neuralgia, along with reducing opioid use as compared to lidocaine and placebo16
Bottom Line
These and many other research findings suggest that BoNTA may be a beneficial treatment for treating certain kinds of neuropathic pain which involve neurogenic inflammatory mechanism. Some of the chronic pain conditions that can be treated through BoNTA include postherpetic neuralgia, complex regional pain syndrome, chronic migraines/headaches, painful diabetic neuropathy, arthritis, overactive bladder etc. Many research studies are on-going to examine the effects of botox in treating other prominent pain conditions.
Refernces
[1] Smuts, Johan A.; Schultz, Donovan; Barnard, Adri. “Mechanism of Action of Botulinum Toxin Type A in Migraine Prevention: A Pilot Study.” Headache: The Journal of Head and Face Pain. 44.8 (September 2004): 801-805. Print.
[2] Oliver, M., MacDonald, J., & Rajwani, M. (2006). The use of botulinum neurotoxin type A (Botox) for headaches: a case review. The Journal of the Canadian Chiropractic Association, 50(4), 263–270.
[3] Aoki, K. R. (2003), Evidence for Antinociceptive Activity of Botulinum Toxin Type A in Pain Management. Headache: The Journal of Head and Face Pain, 43: 9–15. doi:10.1046/j.1526-4610.43.7s.3.x
[4] https://www.ncbi.nlm.nih.gov/pubmed/12887389
[5] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3306767/
[6] Durham, P. L. (2006). Calcitonin Gene-Related Peptide (CGRP) and Migraine. Headache, 46(Suppl 1), S3–S8.
[7] Durham, P. L., & Masterson, C. G. (2013). Two Mechanisms Involved in Trigeminal CGRP Release: Implications for Migraine Treatment. Headache, 53(1), 67–80. http://doi.org/10.1111/j.1526-4610.2012.02262.x
[8] Wu, C., Xie, N., Lian, Y., Xu, H., Chen, C., Zheng, Y., … Zhang, H. (2016). Central antinociceptive activity of peripherally applied botulinum toxin type A in lab rat model of trigeminal neuralgia. SpringerPlus, 5, 431. http://doi.org/10.1186/s40064-016-2071-2
[9] Bach-Rojecky L, Relja M, Lacković Z. 2005. Botulinum toxin type A in experimental neuropathic pain. J Neural Transm (Vienna). 112(2):215–219.
[10] Aoki KR. Evidence for antinociceptive activity of botulinum toxin type A in pain management. Headache. 2003 Jul-Aug;43 Suppl 1:S9-15.
[11] Durham, P. L., & Cady, R. (2011). Insights Into the Mechanism of OnabotulinumtoxinA in Chronic Migraine. Headache, 51(10), 1573–1577. http://doi.org/10.1111/j.1526-4610.2011.02022.x
[12] Pellizzari R., Rossetto O., Schiavo G., Montecucco C. Tetanus and botulinum neurotoxins: Mechanism of action and therapeutic uses. Philos. Trans. R. Soc. Lond. B Biol. Sci. 1999;354:259–268. doi: 10.1098/rstb.1999.0377
[13] Mense S. Neurobiological basis for the use of botulinum toxin in pain therapy. J. Neurol. 2004;251:I1–I7. doi: 10.1007/s00415-004-1102-z.
[14] Oh, H.-M., & Chung, M. E. (2015). Botulinum Toxin for Neuropathic Pain: A Review of the Literature. Toxins, 7(8), 3127–3154. http://doi.org/10.3390/toxins7083127
[15] Ranoux, D., Attal, N., Morain, F. and Bouhassira, D. (2008), Botulinum toxin type a induces direct analgesic effects in chronic neuropathic pain. Ann Neurol., 64: 274–283. doi:10.1002/ana.21427
[16] Xiao, L., Mackey, S., Hui, H., Xong, D., Zhang, Q. and Zhang, D. (2010), Subcutaneous Injection of Botulinum Toxin A Is Beneficial in Postherpetic Neuralgia. Pain Medicine, 11: 1827–1833. doi:10.1111/j.1526-4637.2010.01003.x
Dr. A. Farhan Haq
Related Posts
We use cookies to give you the most relevant experience, Cookie Policy.
See What Our Fellows Have Been Up to Recently
Historically, aspirating before administering certain injections, especially intramuscular ones, was standard practice. The main reason for aspiration was to avoid injecting medication directly into the bloodstream, which could cause adverse reactions or reduce the effectiveness of the medication.
However, the necessity and relevance of this practice have been debated in recent years. Some recent guidelines and studies suggest that aspiration may not be necessary for all types of injections. For example, it’s generally agreed that aspiration is not required for subcutaneous injections because there are fewer large blood vessels in the subcutaneous tissue that could be accidentally punctured. For intramuscular injections, the necessity of aspiration might depend on the injection site. For instance, aspiration is still recommended by some for injections in areas where large blood vessels are present, but it might be considered unnecessary for other sites.
The shift in practice is partly due to a better understanding of anatomy and the low risk of injecting into a blood vessel in certain areas, along with a desire to streamline the injection process and reduce patient discomfort. However, opinions and practices vary, with some healthcare professionals continuing to advocate for aspiration as a precautionary measure, while others view it as an unnecessary step for most injections.
#aestheticmedicine #dermalfiller #aceconference

Understanding depth, volume, and pressure can enhance a practitioner’s skill set, enabling them to provide more valuable services to their clients using their existing tools. #aestheticmedicine #dermalfillertraining #wrinklefree

Mastering hand stability isn’t magic, it’s a mix of experience & targeted learning 🎯 Our students get ahead with specialized techniques, paving the way for precise injections! 💉#SkillDevelopment #FutureHealthPros
.
.
.
.
.
#dermalfillertraining #aestheticmedicine #botoxtraining

Virtually any area can be reached using a cannula #fillertraining #aestheticmedicine #hsifellowprogram

“Unlock Your Aesthetic Potential with Harley Street Institute’s Fellowship! 🌟 Elevate your skills in aesthetic medicine through our intensive hands-on training in Botox and Dermal Fillers. Get ready to sculpt beauty, one injection at a time! 💉✨ Join us for a transformative learning journey that takes you beyond the classroom and into real-world expertise. Are you ready to master the art of enhancing natural beauty? 💫 #HarleyStreetFellowship #AestheticMedicineMastery #SculptingBeauty”

Link in bio
"Unlocking the Secrets of Masseter Botox: Empowering smiles, one injection at a time! 💉💪 Join me on an exciting journey as we delve into the world of Masseter Botox. Learn the art and science behind this transformative procedure, and discover how it can redefine facial aesthetics. Don`t miss out on this opportunity to enhance your skills and expand your practice. Let`s reshape faces and build confidence together!
Link in bio.
#MasseterBotoxCourse #FacialAesthetics #TransformativeProcedures #SmileEnhancement #ContinuingEducation
#aestheticmedicine

💭Have You Ever thought :
👉🏼What lies beneath the orbicularis oculi ?
👉🏼Why do I need to have the correct depth ?
👉🏼How to avoid an asymmetric smile, periorbital edema or a shelf like look at the lid/cheek junction ?
⚠️We all know that when treating crows feet, we are administering botox into the orbicularis oculi, and that there are complications but which and how?
‼️Too inferior or deep🟰 an asymmetric smile
(you’ve hit the zygomaticus minor muscle and major if you’re really too inferior!)
‼️Too medially 🟰 periorbital edema
(and you’re the periorbital region )
Located just underneath the skin, the orbicularis oculi has multiple origin and insertion points. A paired muscle, that overlies the periorbital region in a circular manner.
⚠️The wrong location, the wrong depth can result you injecting botox into a completely different muscle.

Welcome to the under eye region, an area of the face that can often show signs of aging such as wrinkles, hollows, and dark circles. Today, I want to share with you how fillers can be used to address these concerns by injecting them into different layers of the skin.
Using a needle, we can inject fillers into the dermis layer of the skin to improve the appearance of fine lines and wrinkles. This can help to smooth out the texture of the skin and create a more youthful and refreshed look. However, it’s important to note that injecting fillers into this layer requires specialized training and experience to ensure safe and effective results.
In addition to the dermis layer, fillers can also be injected into the bone to help address deeper hollows and shadows under the eyes. This technique requires a higher level of expertise as it involves precise placement of the filler to achieve the desired outcome.
Lastly, fillers can be injected into the fat compartment of the under eye region using a cannula. This method can help to add volume and smooth out any irregularities in the fat pads under the eyes. Again, specialized training and experience are crucial for safe and effective results.
Overall, the use of fillers in the under eye region can provide a non-surgical solution to address signs of aging and enhance the appearance of the face. However, it’s important to seek out a qualified and experienced provider who has received proper training in the use of fillers in this delicate area.
If you’re interested in learning more about how fillers can benefit you, please don’t hesitate to reach out and schedule a consultation. Let’s work together to help you achieve your aesthetic goals!
#cosmedocs #harleystreetinstitute
.
.
.
.
#lifestyleblogger
#selfcarematters #aestheticmedicine
#beautytips
#skincarecommunity
#antiagingtips
#makeuptutorials
#selfcarelove
#aestheticbeauty
#lifestyleinspo #lifestyleblogger
#selfcarematters #dermalfillertraining
#beautytips
#skincarecommunity
#antiagingtips
#makeuptutorials
#selfcarelove #dermalfillers
#aestheticbeauty
#lifestyleinspo
#antiagingsecrets
#harleystreet #drahmedhaq #oxforduniversity
#harleystreetinstitute

The mentalis muscle is a facial muscle located in the chin area. It originates from the mandible and extends downward to the skin of the chin. The primary function of the mentalis muscle is to control the movement and position of the lower lip and the skin of the chin. It plays an important role in activities such as speaking, smiling, and pouting.
In addition to its role in facial expression, the mentalis muscle also helps to maintain the position of the lower front teeth and the shape of the lower lip. Dysfunction or hyperactivity of the mentalis muscle can lead to the development of chin wrinkles, which are vertical lines that appear on the skin of the chin. Understanding the anatomy and function of the mentalis muscle is important for healthcare providers when performing aesthetic procedures in the chin area.
Online Course With Video Demo
www.harleystreetinstitute.com
#botoxtraining #mentalistreatment

#Repost @dranabilamzavala with many thanks 🙏 and best wishes for the future.
Esta semana tuve la oportunidad de estar en Londres en una de las mejores clínicas con los mejores equipos de Medicina Estética en el mundo, perfeccionado técnicas de Rinomodelación con el Dr.Ahmed Haq.
——
@drahmedhaq You are simply incredible, thanks for the hands on and all the new techniques you shared. @drahmedhaq @harleystreetinstitute @cosmedocs
.
.
.
#aestheticmedicine #dermalfillertraining #nosejob #medicaltraining #plab #harleystreet #10harleystreet #aesthetics

Huge Congratulations to Mariana, on completing her foundation course in Aesthetics Medicine with us here at Harley Street Institute. 🥇✨
This combined course covers the necessities required for daily clinic practise, whether starting out or refreshing skills. Our small group training (4:1) provide unparalleled mentorship at any of our training days.
#cosmetictraining #aesthetics #hsi #cosmetics #cosmedocs #harleystreetcourses #foundationcourse #london

Only courses with true mentorship. #botoxtraining #dermalfillertraining #aestheticmedicine #hsifellowprogram #harleystreetfellowship

Huge congratulations to @onemedicalclinic for completing her Fellowship in aesthetic Medicine with us at Harley Street Institute 💫💫✨ We are so proud of having you 🥰
#Repost
Dr Crystal:”When I completed medical school 13 years ago, one of my cherished mentors gave me advice that has stayed with me for life - “never stop learning; it makes the difference between being good and being great."
From my years of Ophthalmic-surgical training to becoming a student of Public Health to my experience as a legislator in Parliament to operating my own
Medical and Aesthetic Medical practice, the lessons learned have been varied and valuable. 🤓
On this occasion my commitment to lifelong learning led me to Harley Street, London. I didn’t just want to be a good injector, I needed to be a great one so I needed to go where the great injectors were. 💉
Every day for the last two months I was immersed in one-on-one intensive training with the aim of mastering my injectable skills and thanks to the incredible team of doctors and trainers at @cosmedocs
@harleystreetinstitute l am proud to say Mission Accomplished! “

Huge Congratulations to Dale Rae for completing the Certificate in Aesthetic Medicine training program. 💫💫
💉The 3-day Aesthetic Medicine Certificate is tailored towards new practitioners who are ready to kick-start their career in Aesthetic Medicine. It aims to provide an in-depth understanding of the Layers of the Skin and Biological Ageing Process. The package also includes our most popular Foundation Botulinum Toxin and Dermal Fillers course, including an introduction to using cannula.
💉It is an Intense 3-day course incorporating essentials basic and advanced botox and dermal filler procedures combined with popular skin treatments perfect for the beginner all-rounded aesthetic practitioner.
You will be provided direct mentorship by our various cosmetic practitioners who are experts in performing their respective aesthetic treatments.
💉Small group training under the direct supervision of our experienced aesthetic trainers. Master procedures to an advanced level. Learn theory, consultation methods and manage client expectations as well as complications.
🙌 DM for more details. #aesthetic #dermalfillers #detmalfillertraining

Aesthetic medicine is an art. It`s not enough to know facial anatomy or to be a good injector. The best aesthetic doctor has an artistic eye. Sometimes this is a skill that can be developed over years. Being able to assess a fa ce within seconds of walking into a room. Knowing exactly how injectables can be used for subtle and natural results.
The end result should not be obvious to an untrained eye.
It`s such a shame to see overfilled faces exaggerating proportions. When really, the main aims are to restore volume lost or correct natural imbalances.
#aestheticmedicine #dermalfillers #beauty
Repost @cosmedocs

Huge Congratulations to @erikatydermatology for completing her Fellowship in Aesthetic Medicine with us at the Harley Street Institute 💫💫💫
Our Aesthetic Fellowship is the pinnacle of training for those seriously interested in escalating their careers.
.
Our fellows are taken on board within clinic over 3 months with weekend workshops, 1-1 mentoring, treatment log book and clinical assistance.
.
Following on from this they have the opportunity to have Independent Fellow Clinics to improve their confidence with patient consultation and individual treatment planning.
.
We believe that this is the future of aesthetic traning to ensure that practitioners have captured all the essential skills for successful careers.
.
We have been extremely proud of our old fellows, many who have moved on to now work with some of the most prestigious clinics in London.
.
Next enrolment periods: TBC
.
To find out more information or to apply, please email your CV to [email protected]
.
#thefellowship #harleystreetinstitute #doctorsanddentists








Note: if you did not get the email, please check spam/junk folder